#do my nursing assignment
Text
Reliably Rescued: A Student's Gratitude for NursingAssignmentHelp.com

As a nursing student, grappling with complex assignments became a daunting task. The intricate details of medical scenarios and the demand for precision in nursing assignments left me feeling overwhelmed. That's when I stumbled upon NursingAssignmentHelp.com, and it was nothing short of a lifesaver.
I was desperately seeking Help with nursing assignments when I discovered this reliable platform. The problem of deciphering medical jargon and presenting it coherently in assignments seemed insurmountable. However, the moment I reached out to NursingAssignmentHelp.com, I knew I had found a trustworthy ally. Their services spanned a spectrum of nursing topics, from pharmacology to patient care, providing comprehensive assistance.
Availing their services was a breeze. The user-friendly interface allowed me to upload my assignment details effortlessly. The process was transparent, and their commitment to deadlines was commendable. The reliability of their team became evident when they not only met but exceeded my expectations. The quality of the content was exceptional, showcasing their in-depth understanding of nursing concepts.
I am incredibly grateful for stumbling upon NursingAssignmentHelp.com at the right time. Their reliability, professionalism, and commitment to excellence turned my academic challenges into victories. If you find yourself drowning in nursing assignments, don't hesitate to seek help from this reliable platform. It's a decision you won't regret.
#Nursing Assignment Help#Help with Nursing Assignments#Do My Nursing Assignment#Complete My Nursing Assignment
5 notes
·
View notes
Text

How do my nursing assignment kind of services beneficial for Students?
#do my nursing assignment#Nursing assignment#nursing assignment Australia#Pay someone to do my assignment
1 note
·
View note
Text

#nursing assignment help#nursing assignment#nursing homework help#do my nursing assignment#Nursing Assignment Writing
0 notes
Text
If you need help with a nursing assignment, visit www.nursingassignmenthelp.com. They have a large number of nursing expert. Nursing Assignment Help provides the best help for assisting students to complete their assignments ahead of schedule and get the best grades as per exact specifications.
Their team is always ready to help with all nursing, medical and midwifery tasks. Their dedicated team provides great tutoring to help you remember everything in class.
Contact [email protected] or visit www.nursingassignmenthelp.com for help in assigning the best nursing care.
#Do My Nursing Assignment#Take My Nursing Class for Me#Nursing Assignment Helper#Nursing Dissertation Help#Take My Nursing Exams#education#science#student#teaching
1 note
·
View note
Text


Moon 2.
#skuaclan#warrior cats ocs#note 1: i mixed up which of foxfern's sides was grey whoops. i blame the weird perspective#note 2: when i say 'their' i just mean the loner! they're not cinder's. their parent was a stranger to him. (their name was procyon)#ravenkit#fogkit#foxfern#sunstar#bluekit#cinderplume#note 3: ive ambiguously aged up these kittens a bit for lore purposes to the extent where they can be weaned. so dont worry about it#theyre supposed to be newborns at this point ingame but the difference shouldn't really matter#i cannot be arsed doing a bunch of work to explain skuaclan finding an external nursing queen to temporarily feed them sorry lmfao#also i am assigning them pronouns out the womb so i dont gotta do it later on. @ ravenkit woe he/they be upon ye#if a cat changes gender later on i will account for that obv but im willing to let assumedly cis cats like raven and fox have bonus pronoun#just like. at random. if it seems an arbitrary good fit for the character i begin building in my brain#moonskip events
60 notes
·
View notes
Text
How Does The Brain Work?

The brain stands as a marvel of biological engineering, Composing of a multitude of bodily functions ranging from cognition and memory to emotions and sensory perception. Together with the spinal cord, it constitutes the central nervous system (CNS), the command center of the human body.
Composition of the Brain
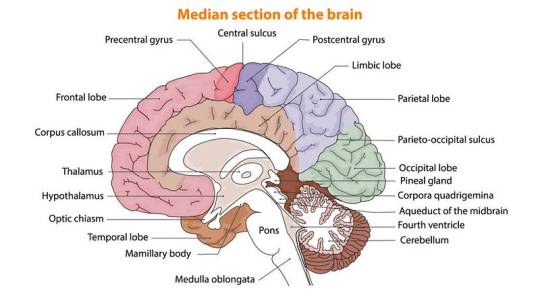
Weighing approximately 3 pounds in adults, the brain’s main structure comprises about 60% fat, interspersed with water, protein, carbohydrates, and salts. Unlike muscles, it houses a complex network of blood vessels and nerves, including neurons and glial cells.
a) Gray and White Matter
Within the central nervous system, gray matter and white matter occupies distinct regions. In the brain, gray matter forms the outer layer, rich in neuron somas, while white matter constitutes the inner section, primarily composed of axons unsheathed in myelin. Conversely, in the spinal cord, this arrangement is reversed.
b) Brain Functionality
The brain operates by transmitting and receiving chemical and electrical signals throughout the body. These signals regulate a myriad of processes, with the brain disseminating each input. Some signals remain confined within the brain, while others traverse the spinal cord and nerves, disseminating information across the body’s expanse. This composes neural network relies on billions of interconnected neurons.
Major Brain Regions and Their Functions
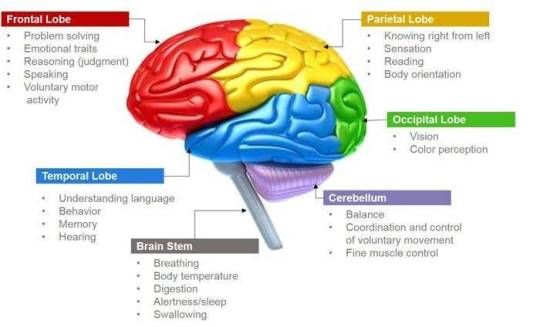
1.Cerebrum
Dominating the brain’s landscape, the cerebrum encompasses the cerebral cortex and underlying white matter. It governs a spectrum of functions, including motor coordination, temperature regulation, language processing, emotional regulation, and sensory perception.
2. Brainstem
Serving as the bridge between the cerebrum and spinal cord, the brainstem comprises the midbrain, pons, and medulla. It regulates vital autonomic functions such as heart rate, breathing, and reflexive responses.
3. Cerebellum
Nestled at the posterior aspect of the brain, the cerebellum coordinates voluntary muscle movements, posture, balance, and motor learning.
Brain Coverings
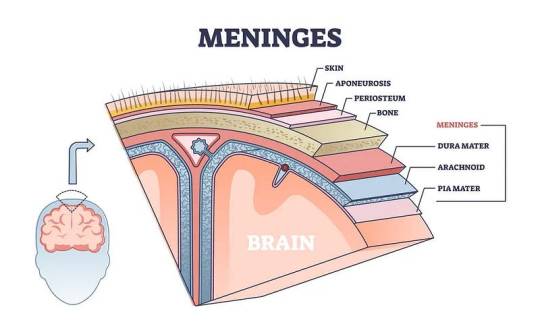
a) Meninges
Three layers of protective membranes, collectively known as meninges, enshroud the brain and spinal cord. These layers — dura mater, arachnoid mater, and pia mater — shield the delicate neural tissue from physical trauma and infection.
b) Lobes of the Brain
Each hemisphere of the brain comprises four lobes, each harboring distinct functional domains:
Frontal Lobe: Governing executive functions, motor control, and higher cognitive processes.
Parietal Lobe: Integrating sensory information, spatial awareness, and perception of pain and touch.
Occipital Lobe: Specialized for visual processing and perception.
Temporal Lobe: Involved in auditory processing, language comprehension, and memory consolidation.
Deeper Brain Structures
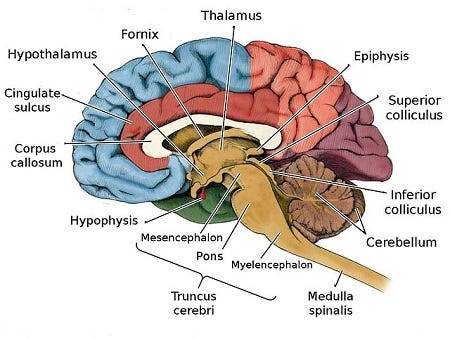
These encompass important structures such as the pituitary gland, hypothalamus, amygdala, hippocampus, and pineal gland, orchestrating hormone secretion, emotional regulation, memory consolidation, and circadian rhythms.
Blood Supply
The brain receives its oxygenated blood supply through the vertebral and carotid arteries, ensuring adequate perfusion of neural tissue. The main network of blood vessels, including the Circle of Willis, safeguards against ischemic insults and facilitates intraarterial communication.
Cranial Nerves
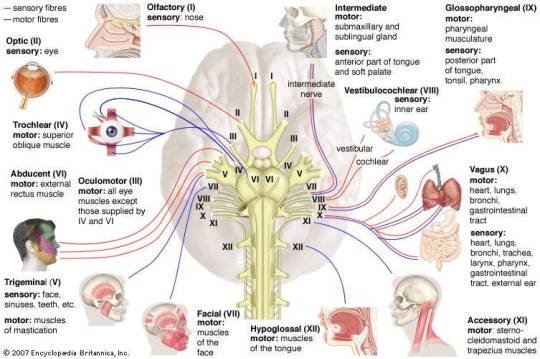
The twelve pairs of cranial nerves, originating from the brainstem, mediate a diverse array of sensory and motor functions, encompassing olfaction, vision, facial expression, and auditory perception.
Comprehending the anatomy and functionality of the brain fosters a deeper appreciation of its complexity and facilitates advances in neuroscientific research and therapeutic interventions aimed at diminishing neurological disorders.
Understanding the detailed anatomy and functionality of the brain is crucial for medical students embarking on their journey of study. Expert Academic Assignment Help offers invaluable assistance in navigating the complexities of neuroscience and related subjects. By leveraging expert guidance and support, students can excel in their medical education and contribute to advancements in the field of Medicine. Email us at [email protected] to embark on your path to scholarly excellence and professional competency.
#studying#studyblr#study blog#study aesthetic#student life#student#medical student#medical school#medicine#university student#university#university life#assignment help#medical students#nursing student#nursing school#healthcare#health and wellness#mental health#psychology#phd life#phd thesis writing service#online writing#do my online class#academic writing#essay writing#academic assignments#academia
10 notes
·
View notes
Text
i always forget i have Healthcare System Anxiety until i have to interact with The Healthcare System and immediately just start screaming internally for days
#my mom obliterated her bones and the pre-surgery surgery post-surgery experience. the ER situation. moving 2 the woods#this is a vent post i forget my complaining tag#waited 30 mins for an ambulance & when we called back they were like ''yeah it hasnt been assigned to anyone & might be hours''#so i drove her to the ER with a migraine & ran over some pylons (cool).#stuck in the ER for 9 hours. took 4 hours for anyone to give her any kind of pain management. i caught covid#was supposed to get a call when she was out of her 2 hrs max surgery. was told i could call if i hadn't heard anything#5 hours later i called and was transferred 6 times - told she had been discharged - told she had never been registered at that hospital -#yelled at by a nurse for asking for patient information - eventually got the right department and was told oh yeah sorry she's in recovery#was supposed to find out if she could come home or not in 30 mins. 3 hours later theyre like OK come get her#i show up and the doors to that wing are. locked? and no one's there to unlock them?#apparently i was supposed to pick up the wall phone? and call a code they hadn't given me? spent 30 mins getting help from other department#to GET THEM TO OPEN THE DOORS. FREE HER RELEASE HER#finally i get in and she's OK SHES FINE except morphine doesn't work on her so that's. fine. bodies are good to have#we have reached shrimp colours levels of anxiety i am a walking talking stress migraine but she's doing ok. but holy fuck#kayvswords#also like she's black and all of her nurses and doctors have been white so feeling normal about all of it all around
25 notes
·
View notes
Text
Either my story post really sucks. Or it doesn't appear on anyone's dash... 'cause even my most useless text posts get notes, but my first part of "Sacrélège"? Just one note (well, two but one is my own rb) since I posted it last evening.
Or everyone decided that I suck and they now hate me.
(yes, I'm in a very confident mood, as you can see)(no I'm not; I kinda want to abandon my new story because it's probably too shitty anyway and just lie in bed for the next decade or so)
#and to help with the self-confidence i still haven't managed to have a new psych nurse assigned to me#since september though i asked them to and they said they would contact me#and even after leaving messages for them to call me i still don't have any answer#my former nurse would have never do that; though now that i think of it she was supposed to call me before she left#but i think her colleague never gave her the message 'cause she always had been awesome and i trust her#so yeah i feel like i'm not wanted#which sucks ass#i'll just go watch dumb movies under my weighted blanket then#i should just shut up
7 notes
·
View notes
Text
the way that i’m trying to care about things but i really don’t give a shit
#i’m still in an anatomy class but i do not careeeee#i’m out of nursing school and my cat just died so i’m honestly really trying#but i just don’t give a fuck#three assignments due at 5 and i don’t care to start any of them
3 notes
·
View notes
Text
#assignmentwriting#college student#online learning#criminal law assignment topics#criminal law assignment examples#help with criminal law assignment#online tutoring#do my criminal law assignment#5cs marketing assignment#cipd assignment examples cipd level 3 cipd level 5 cipd level 7 cipd assignment question and answers cipd essays cipd uk cipd uae cipd leve#assignment help#domyhomework#essayhelp#homeworkhelper#homework helper#summer courses#management courses#nursing courses#IT courses#technical IT papers#exams#quizzes#quick quizzes
3 notes
·
View notes
Text
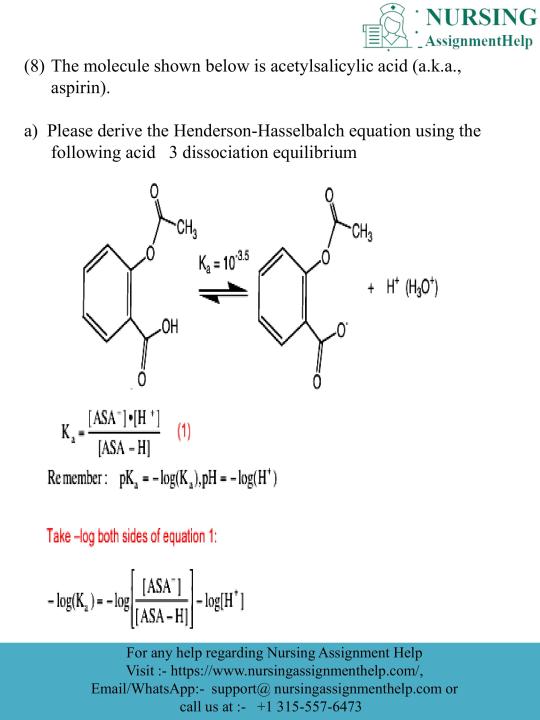
Do My Nursing Assignment
If you're a nursing student who is struggling with your assignments, then you've come to the right place! we provide high-quality nursing assignment to students who need it. Our team of expert writers is highly experienced in nursing and can help you complete your assignments with ease. We understand that nursing assignments can be complex and time-consuming, which is why we offer affordable and reliable assistance to ensure that you meet your academic goals.
Our writers are dedicated to providing you with the best possible service, and we guarantee that you will be satisfied with the results. So if you're looking for someone to "do my nursing assignment", look no further. We're here to help you succeed!
Submit your order at [email protected] or call/WhatsApp at +1(315)557–6437.

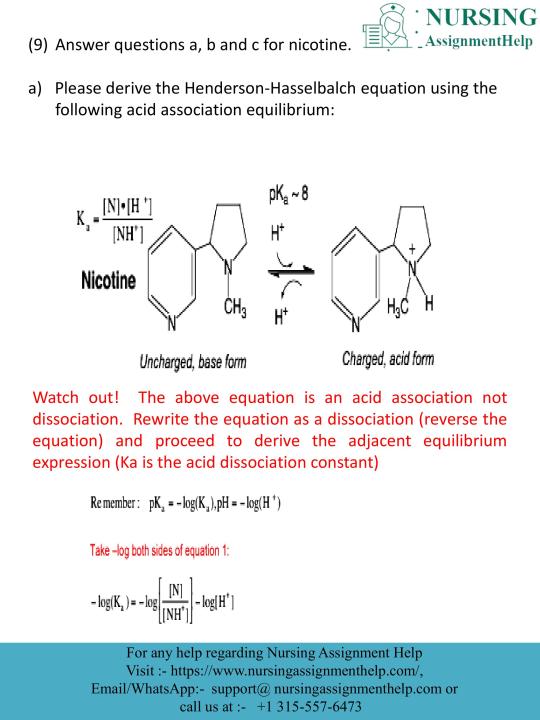

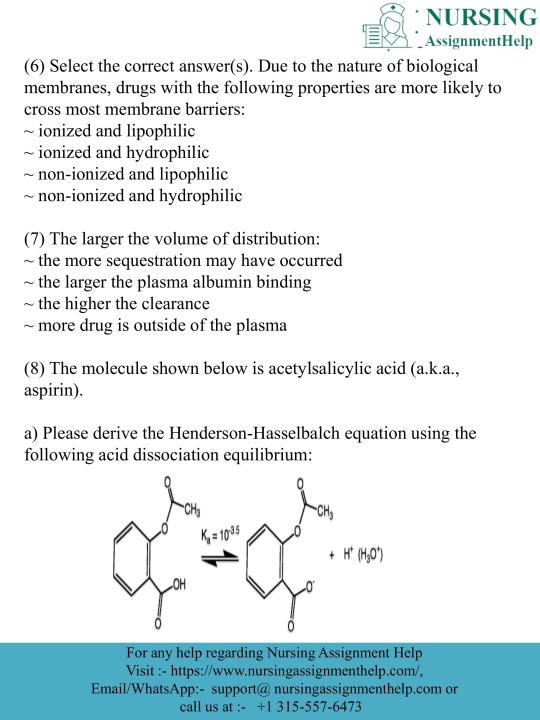







#Do My Nursing Assignment#education#University#study tips#Assignment Sample#Educational Website#nursing student#Assignment Help#Academic#Tutor
0 notes
Text

Are you Searching for “do my nursing assignment”? Get Expert Help Today
0 notes
Text
Hire me for Personalized & Affordable Expert Help in any Coursework this Semester. Payment only on Delivery || 100% Original Work || Plenty of Samples Available on Request || 24/7 Support
If you need help in any one of the following areas, then I'm your go-to guy.
> Essays, research papers, discussion posts, and/or assignments in Sociology, Psychology, Business & Management, Religion, Computer Science & IT, Nursing & Health Sciences, Law, Political Science, History, English & Literature, Gender & Diversity Studies, Math, Physics, and STEM.
> Descriptive, Expository, Persuasive, Argumentative, Analytical, Compare & Contrast essays in the above mentioned subjects.
> General Research Papers, Annotated Bibliographies, Term Papers, Discussion Boards, Speech Writing and Analyses, Literature Reviews, Thesis, Dissertations, and Case Studies.
> Front End Web Development (HTML, CSS, JavaScript).
Every Hire Guarantees you the Following:
1. Excellently formatted papers in any citation style (MLA, APA, Harvard, Chicago/Turabian, Vancouver, AMA, etc.) at no extra cost.
2. Free Abstracts, Title Pages, Reference/Bibliography Pages, Table of Contents, and List Figures & Abbreviations.
3. 100% Original Papers, crafted carefully from scratch with free Turnitin reports.
4. Free revisions and/or adjustments until you are 100% satisfied.
5. Free-flowing natural English as your papers/ assignments will be written/done by native English Speakers in the US.
6. Excellently structured essays with glowing introductions, memorable thesis statements, logically flowing body paragraphs, and carefully crafted, fresh conclusions that will earn you a top grade.
7. Use of reputable databases for research.
Contact me now for an incredible deal.
Email: [email protected]
Discord: Profsocrates#0762
Text: +1 (508) 738-7180
Most welcome!
#study#college#students#help with criminal law assignment#examination#do your homework#assignmentwriting#assignment help#university#writing#writerscommunity#writers on tumblr#academic writing#academic work#lazy writing#do my essay#do my assignment#nursing assignment writers#nursing assignment help#college life#nursing assignment writing#persuasive essay#essayhelp#custom essay paper#academic essay#college essay#college student#high school students#education#colleges
12 notes
·
View notes
Text

Nursing assignment help is an excellent way for students to maintain good grades as they complete their assignments on time. They can use these services to get assignments done on time and enjoy the rest of their life.
#nursing assignment help#nursing assignment#nursing homework help#nursing homework assignments#nursing assignment expert#do my nursing assignment#Nursing Assignment Writing#write my nursing assignment
0 notes
Text
My mom wondering what me and the doctor are saying about my fucked up arm:
Me and the doctor talking about anime:
#clown hours#she was disappointed in me#but jokes on her#every time I go to an appointment someone ends up talking to me about anime#even during the surgery#but it’s funny#they do it cause I wear anime t shirts to my appointments since it’s easy to put on for my arm#but so far I’ve talked to the dude who took out my stitches about anime#and to the nurse assigned to me during surgery#and to the doctor himself 💀
6 notes
·
View notes
Text
The Pathophysiology Of Spondylitis
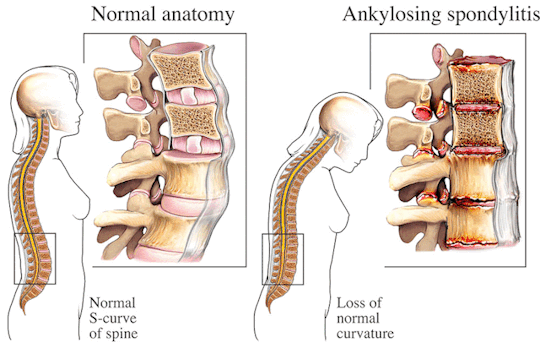
Spondylitis is a comprehensive term used to describe a group of chronic inflammatory diseases that primarily affect the joints of the spine and the sacroiliac region, which includes the pelvis and lower spine. These conditions are characterized by arthritis-like symptoms and can lead to significant discomfort, reduced mobility, and other systemic complications. This detailed exploration will indulge into the nature of spondylitis, how it differs from the related condition known as spondylosis, the various types of spondylitis, diagnostic methods, treatment options, and complementary therapies.
What is Spondylitis?
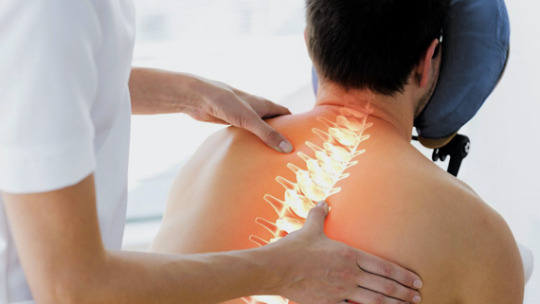
Spondylitis involves inflammation of the joints, tendons, and ligaments within the spine and sacroiliac region. Tendons are connective tissues that attach muscles to bones, while ligaments connect bones to other bones. This inflammation can result in the fusion of bones (ankylosis) and the formation of new bone, leading to stiffness and reduced flexibility in the spine. In severe cases, excessive bone growth can cause significant curvature of the spine, known as kyphosis.
Spondylitis vs. Spondylosis
While both spondylitis and spondylosis cause pain in the hip and back, they are distinct conditions with different etiologies and characteristics.
Spondylitis is an autoimmune disorder where the immune system mistakenly attacks the joints, causing inflammation, bone fusion, and excessive bone formation. This condition typically develops in teenagers and young adults and can affect multiple organs and systems within the body.
Spondylosis, on the other hand, is a degenerative condition associated with aging and the natural wear and tear of the spine. It involves the degeneration of spinal joints and discs, often accompanied by the formation of bone spurs (osteophytes). Spondylosis primarily affects older individuals, with more than 85% of people over the age of 60 experiencing this condition.
Types of Spondylitis
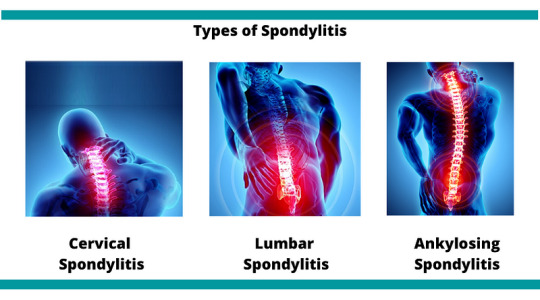
Medical professionals categorize spondylitis using two primary classification systems: the traditional system and the newer system. The traditional system recognizes six specific types of spondylitis, whereas the newer system categorizes spondylitis into two broad types based on the affected body region.
Traditional Spondylitis Classifications:
a) Ankylosing Spondylitis (AS)
Symptoms: Ankylosing spondylitis primarily affects the spine, causing symptoms such as fatigue, chronic back pain, stiffness, and inflammation in various areas of the body, including joints and tendons. Over time, the vertebrae may fuse, leading to reduced mobility and flexibility.
Causes: The exact cause of AS is unknown, but a strong genetic association exists with the HLA-B27 gene. Approximately 90% of individuals with AS carry this gene, although not all carriers develop the disease.
b) Reactive Arthritis
Symptoms: Reactive arthritis typically presents with a triad of symptoms including arthritis (swelling and pain in joints), conjunctivitis (inflammation of the eyes with a sticky discharge), and urethritis (genital and bladder inflammation with painful urination). However, not all patients exhibit all three symptoms.
Causes: often follows a gastrointestinal infection or a sexually transmitted infection (STI). The immune system overreacts to the initial infection, leading to inflammation and joint pain. The HLA-B27 gene is also strongly linked to ReA, with 30–50% of affected individuals carrying this gene.
c) Psoriatic Arthritis (PsA)
Symptoms: Psoriatic arthritis is associated with the inflammatory skin condition psoriasis. Symptoms include dactylitis (swelling in toes and fingers), changes in nails (such as pitting), eye pain, joint pain, reduced range of motion, and fatigue. PsA typically affects people aged 30–50.
Causes: PsA often follows psoriasis, but it can also develop in individuals without skin symptoms. There is a genetic predisposition to PsA, with at least 10% of the population inheriting genes that increase susceptibility to psoriasis and PsA.
d) Enteropathic Arthritis (EnA)
Symptoms
Enteropathic arthritis is linked to inflammatory bowel diseases (IBDs) such as ulcerative colitis and Crohn’s disease. Symptoms include abdominal pain, bloody diarrhea, and joint swelling and pain.
Causes
The precise cause of EnA is unclear, but it is associated with chronic inflammation in the bowel. This inflammation may allow bacteria to penetrate the bowel wall, triggering an immune response that leads to joint inflammation. The HLA-B27 gene is also linked to EnA.
d) Juvenile Spondyloarthritis (JSpA)
Symptoms
Juvenile spondyloarthritis begins in individuals aged 16 or younger and typically affects the leg joints. Symptoms include joint pain, tenderness, and bowel inflammation.
Causes
Similar to adult spondylitis, JSpA is often associated with the HLA-B27 gene. The exact cause remains unknown, but genetic and environmental factors likely play a role.
e)Undifferentiated Spondyloarthritis (USpA)
Symptoms
USpA is characterized by a variety of symptoms that do not fit neatly into a specific rheumatoid disorder. Symptoms may include persistent lower back pain, joint pain in small and large joints, heel pain, swelling in hands and feet, general stiffness, eye inflammation, rash, urinary tract symptoms, and intestinal inflammation.
Causes
The causes of USpA are diverse and not fully understood. It encompasses a range of symptoms that do not meet the criteria for other specific types of spondylitis.
Newer Spondylitis Categorizations
Peripheral Spondyloarthritis (pSpA)
Peripheral spondyloarthritis affects joints and tendons outside the spine and sacroiliac joints, such as the hands, wrists, elbows, shoulders, knees, ankles, and feet. It includes forms of spondylitis such as reactive arthritis, enteropathic arthritis, and undifferentiated arthritis.
2. Axial Spondyloarthritis (AxSpA)
Axial spondyloarthritis involves inflammation and pain in the pelvis and spine. This category covers a broad range of spondylitis types and includes individuals with and without sacroiliac joint fusion. AxSpA is further subdivided into non-radiographic AxSpA (without visible joint damage on X-rays) and radiographic AxSpA (visible joint damage).
Diagnosis
Diagnosing spondylitis involves abroad approach, combining physical examination, medical history, and various diagnostic tests. There is no single definitive test for spondylitis, making a comprehensive evaluation essential.
a) Physical Examination
During a physical examination, the doctor will assess the patient’s symptoms, medical history, and family history of autoimmune diseases such as psoriasis and spondyloarthritis. The examination may include evaluating joint tenderness, swelling, and range of motion.
b) Diagnostic Tests
Blood Tests: Blood tests can help identify markers of inflammation, such as elevated erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP). Testing for the presence of the HLA-B27 gene can also provide valuable information, although not all individuals with spondylitis carry this gene.
Imaging Tests: Imaging techniques are crucial for diagnosing spondylitis and assessing the extent of joint and bone damage.
X-rays: X-rays can reveal changes in the spine and sacroiliac joints, such as joint fusion and bone spurs.
MRI Scans: MRI scans provide detailed images of soft tissues and can detect early signs of inflammation and joint damage that may not be visible on X-rays.
Ultrasound Scans: Ultrasound scans can be used to assess inflammation in peripheral joints and tendons.
Genetic Testing: Testing for the HLA-B27 gene can support the diagnosis, particularly in cases where clinical symptoms and imaging findings are inconclusive.
Treatment
While there is no cure for spondylitis, various treatments can help manage symptoms, reduce inflammation, and improve the patient’s quality of life. Treatment plans are often tailored to the individual’s specific symptoms and disease severity.
Medications
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): NSAIDs are commonly used to reduce inflammation and pain in spondylitis patients. Examples include ibuprofen and naproxen.
Corticosteroids: Corticosteroids, such as prednisone, can be prescribed for short-term use to control severe inflammation and pain.
Disease-Modifying Antirheumatic Drugs (DMARDs): DMARDs, including methotrexate and sulfasalazine, can help manage symptoms and slow disease progression in some types of spondylitis.
Biologic Agents: Biologic agents, such as tumor necrosis factor (TNF) inhibitors (e.g., adalimumab, etanercept) and interleukin-17 (IL-17) inhibitors (e.g., secukinumab), target specific components of the immune system to reduce inflammation and prevent joint damage.
Analgesics: Pain relievers, such as acetaminophen, may be used to manage pain when inflammation is not the primary issue.
Physical Therapy
Physical therapy plays a crucial role in managing spondylitis by improving and maintaining spine flexibility and overall mobility. Techniques may include:
Massage Therapy: Therapeutic massage can help reduce muscle tension, improve circulation, and alleviate pain.
Spinal Manipulation: Performed by a trained physical therapist or chiropractor, spinal manipulation can enhance mobility and reduce pain.
Exercises: Tailored exercise programs can help strengthen muscles, improve posture, and enhance flexibility. Stretching exercises are particularly beneficial for maintaining spine and joint flexibility.
Breathing Exercises: Breathing exercises are essential for individuals with ankylosing spondylitis, as the condition can affect chest expansion and respiratory function. These exercises help maintain normal lung function and prevent restrictive lung disease.
Surgery: Surgery is generally considered a last resort and is reserved for severe cases where conservative treatments have failed. Surgical options include:
Joint Replacement: For patients with severe joint damage, joint replacement surgery (e.g., hip or knee replacement) can restore function and relieve pain.
Spinal Surgery: In cases of severe spinal deformity or nerve compression, spinal surgery may be necessary to correct curvature and alleviate pressure on nerves.
Complementary Therapies
In addition to conventional treatments, complementary therapies can provide additional symptom relief and improve overall well-being. These therapies are often used alongside standard medical treatments.
Massage Therapy: Massage therapy can help reduce muscle tension, improve blood circulation, and alleviate pain and stiffness in the affected areas.
Relaxation Techniques: Techniques such as deep breathing, progressive muscle relaxation, and meditation can help manage stress and reduce pain perception.
Yoga: Yoga combines physical postures, breathing exercises, and meditation to improve flexibility, strength, and relaxation. Yoga can be particularly beneficial for maintaining spine flexibility and reducing pain.
Acupuncture: Acupuncture involves the insertion of thin needles into specific points on the body to stimulate the nervous system and promote natural pain relief and healing.
Cupping: Cupping is a traditional therapy that involves placing suction cups on the skin to improve blood flow and reduce muscle tension. It can be used to alleviate pain and stiffness in the back and other affected areas.
Summary
Spondylitis encompasses a range of chronic inflammatory diseases that affect the spine and sacroiliac region. It is characterized by autoimmune-driven inflammation, leading to joint pain, stiffness, and potential bone fusion. Spondylitis is distinct from spondylosis, a degenerative condition associated with aging. Medical professionals classify spondylitis into various types based on symptoms and affected body regions. Diagnosis involves a combination of physical examination, medical history, blood tests, imaging, and genetic testing. While there is no cure, treatments such as medications, physical therapy, and complementary therapies can help manage symptoms and improve the quality of life for those affected by spondylitis. By understanding the nature of spondylitis and the available management strategies, individuals can better navigate their condition and maintain an active, fulfilling life.
Medical students and healthcare professionals need to stay informed about the latest advancements in diagnosing and treating spondylitis. Continuous education and expert guidance are crucial for managing these complex conditions. For additional support with challenging medical units, clinical studies, research projects, assignments, and exam preparation, Expert Academic Assignment Help offers professional resources and online classes. For personalized assistance, contact [email protected] Accessing expert guidance can significantly enhance your understanding and proficiency in medical education.
#medical students#assignment help#nursing school#nursing student#medicine#healthcare#student life#medical student#studyblr#case study#student#online writing#do my online class#essay writing#phd research#clinical research#research#phd thesis writing service#phdjourney#phd life#phdblr#studying#study blog#study motivation#studyspo#study aesthetic
4 notes
·
View notes