#dermatomyositis
Text
health update--sorry for doing so much of these, but it’s keeping me sane.
SO. it turns out that I didn’t get this new disease/diagnosis BECAUSE of covid, but it got much worse because of covid--which allowed my rheums to finally diagnose it (AFTER TEN YEARS RIP). dermatomyositis is really difficult to diagnose mostly because it’s so damn rare; what I read was that like 40-90 people in a MILLION get it (or, at least, are diagnosed ...), so most drs aren’t very familiar with it & don’t look for it.
I can’t believe it, tho. after 10 years ... I finally know what the fuck is up w/ my body. -__- so much of drs just “giving up” on my symptoms bc they’re like “idek what’s wrong with you, maybe you’re just weak/unlucky/got a weird kind of eczema, who knows, lol?” ... it was actually this disease. jesus.
#I'm going to research the hell out of this#and annoy my drs so much I don't even care#dermatomyositis#myositis#goddamn does anyone here have this ??#this whole time I've been out in the sun ... rip#well now that it's worse I know what to watch out for#nan.text#heath stuff
5 notes
·
View notes
Text
I remember learning about dermatomyositis, but I don't remember learning that it's associated with ovarian, cervical, lung, pancreatic, bladder, and gastric cancer. You should do age-appropriate cancer screening in pts presenting with dermatomyositis.
Dermatomyositis is an idiopathic inflammatory myopathy that presents with a combination of proximal muscle weakness accompanied by various cutaneous signs. Cutaneous findings can include a reticular, violaceous rash over the back and shoulders (shawl sign), similar lesions over the small joints of the hands (Gottron papules), and periocular patches (heliotrope rash). These rashes are often pruritic and the pruritis itself can be disabling. It is important to recognize that multiple cancers have been associated with the development of DM, and all patients with new DM should be evaluated for underlying malignancy. Cervical, lung, pancreatic, bladder, and gastric cancer account for up to 70% of underlying cancers. Aside from the spectrum of findings attributed to DM, the majority of cancers are otherwise asymptomatic at the time of diagnosis.
Screening tests, ideally, are guided by presenting signs and symptoms. However, in an asymptomatic patient with no other significant risk factors, testing should begin with age-appropriate cancer screening.
Notably, other studies have suggested that the test most likely to reveal an underlying malignancy may be a computed tomography (CT) scan of the chest, abdomen, and pelvis, and this can be considered if age-appropriate cancer screening is unremarkable. Multiple unique clinical syndromes or findings are associated with underlying malignancy.
Bottom Line: Dermatomyositis is associated with an increased incidence of cancer. All patients with a new diagnosis should undergo age-appropriate cancer screening. Select other laboratory tests can be considered as noted above.
COMBANK Insight: An astute clinician can seem a hero when he or she recognizes one of many characteristic cutaneous manifestations associated with systemic neoplasms or syndromes. Knowing the organs potentially involved or diseases is paramount in early and appropriate screening. While select cancers have been shown to be overrepresented in patients with dermatomyositis, the association with ovarian cancer is frequently presented across multiple tests through medical school and residency.
7 notes
·
View notes
Photo

A very special person reminded me that March is also Autoimmune Disease Awareness Month. Kick a$$, everyone! You're rock stars! #AutoimmuneDiseaseAwareness #WhatDoYouKnow #RhuematoidArthritis #MultipleSclerosis #AddisonDisease #CeliacDisease #Dermatomyositis #Lupus #Type1Diabetes #NotAllHandicapsAreVisible #DontBeADick #BeKindHumans https://www.instagram.com/p/CpTU9pevl8-/?igshid=NGJjMDIxMWI=
#autoimmunediseaseawareness#whatdoyouknow#rhuematoidarthritis#multiplesclerosis#addisondisease#celiacdisease#dermatomyositis#lupus#type1diabetes#notallhandicapsarevisible#dontbeadick#bekindhumans
2 notes
·
View notes
Note
Autoimmune culture is getting diagnosed and reading up on it and scaring yourself over the horror stories
Dermatomyositis MDA5 positive gang rise up, our muscles may be failing (especially lungs) because of our immune system, but we didn't fall yet if you can still read this so, good on everyone who is here
My knees hurt, I wanna bawl
i hope you find some relief soon!
8 notes
·
View notes
Text
Logically, I know I shouldn't feel bad that my mom has to go to work while I stay home because I am ill and unable to work. It's not my fault at all. I'm doing the best I can and that is enough. But still, even after 14 years of being chronically ill, there is still the guilt. Less than it once was though.
#my thoughts#chronic illness#chronically ill#spoonie community#spoonie#myosotis#Polymyositis#Dermatomyositis#osteoarthritis#disability#chronically disabled#disabled#chronic illness community
5 notes
·
View notes
Text
I missed my two year anniversary of being diagnosed with my autoimmune condition yesterday.
shout out dermatomyositis for changing the trajectory of my life 2 years ago now!
#mylife#chronic illness#dermatomyositis#like the doctors were suspecting before that but that’s the day it was entered into my files in the hospital!
1 note
·
View note
Text
Dangal actress Suhani Bhatnagar was diagnosed with dermatomyositis, reveal reports
Reports reveal that Suhani had a rash about two months ago, which later resulted in excess fluid being accumulated in her lungs.
The news of the demise of the young Suhani Bhatnagar sent shock waves across the Indian film industry on Saturday. On February 17, after news reports were abuzz about the demise of the teenage star, the reason for this remained mystery. Now, her parents have thrown light on the sudden death of their 19-year-old daughter and revealed that she was suffering dermatomyositis, a rare disease which affected one out of millions in the world.

For the unversed, the Faridabad-based Suhani Bhatnagar was admitted at the All India Institute of Medical Sciences (AIIMS) on February 7. However, her condition worsened which eventually led to her demise, revealed reports. In an interaction with ANI, Suhani’s father Sumit Bhatnagar mentioned that it all started with her developing rash-kind of issues on her skin, which was later diagnosed to be dermatomyositis. But her lungs started failing which eventually led to her demise.
“She developed a red spot on her hands about two months ago. We thought it was allergy and we consulted with doctors in different hospitals in Faridabad but it couldn't be diagnosed. When her condition started deteriorating, we got her admitted to AIIMS. But there was no improvement and her lungs were damaged due to accumulation of excess fluid," he told.
Suhani Bhatnagar catapulted to fame with her debut sports biopic Dangal based on Mahavir Phogat and his daughters, featuring Aamir Khan as Mahavir, Sakshi Tanwar as his wife, Fatima Sana Shaikh as their daughter Geeta Phogat, and Sanya Malhotra as Babita Phogat. Suhani played the younger version of Babita whereas Zaira Wasim played the younger Geeta.
Suhani, however, took a break from acting to complete her studies and was not taking up any acting projects. Her demise left the entire team of Dangal shocked, and Nitesh Tiwari, Aamir Khan Productions and even the real-life sisters Geeta and Babita Phogat shared their condolences to the Bhatnagar family.
#Bollywood#Dangal#Death#Demise#Dermatomyositis#Disease#Health#News#Passed Away#Sickness#Suhani Bhatnagar
1 note
·
View note
Text
In this video, I take you along as I go grab a coffee and a haircut, and then I talk about how my budgeting is going and my fitness goals vs. my current struggles with managing my autoimmune disease (dermatomyositis). I also talk about mood journaling with Mood Chonks and how EMDR is going.
#vlog#day in the life#youtube vlog#EMDR#dermatomyositis#autoimmune disease#budgeting#fitness#chatting video
0 notes
Text
iiiiii am having such a crazy time rn w this flare up and it is so crazy to me that i’ve had these symptoms for like 10 years and had them constantly dismissed because of my mental health history… ? and it sucks that this flare up is so bad but at least finally people are taking me seriously but it sucks that it’s because i’m covered in a full body rash and having trouble breathing and walking and standing and swallowing and everything. anyway. if anyone knows of any resources or groups for ppl w rare diseases/autoimmune diseases/specifically dermatomyositis i would be very interested in learning about it
#also im gonna have to move back to my home city#which is so awesome /s#my mom is definitely going to be normal about it /s#auugughhhhhh. just really fuckin like. weird about this#therapy session gonna go crazy next week#dermatomyositis#autoimmine disease
0 notes
Text
It’s been about 4 years since my original symptoms started. The only autoimmune they thought about was MS or Lupus. They decided it had to be something like Lupus. New symptoms have been occurring this past year and now I’m waiting for results for dermatomyositis. The symptoms fit and the doctor seems to think that she has better meds for me. Fingers crossed that this is the right direction!
0 notes
Text
What is Myositis?
Myositis is the name for a group of rare conditions. The main symptoms are weak, painful or aching muscles. This usually gets worse, slowly over time.
You may also trip or fall a lot, and be very tired after walking or standing. If you have any of these symptoms you should see a GP.
Myositis is usually caused by a problem with your immune system, where it mistakenly attacks healthy tissue.
Types of myositis
There are different types of myositis, including:
Polymyositis, which affects many different muscles, particularly the shoulders, hips and thigh muscles. It's more common in women and tends to affect people aged 30 to 60.
Dermatomyositis, which affects several muscles and causes a rash. It's more common in women and can also affect children (juvenile dermatomyositis).
Inclusion body myositis (IBM), which causes weakness in the thigh muscles, forearm muscles and the muscles below the knee. It may also cause problems with swallowing (dysphagia). IBM is more common in men and tends to affect people over 50.
The UK charity Myositis UK has more information about the different types of myositis.
This page covers polymyositis and dermatomyositis, which are the 2 most common types.
Symptoms of polymyositis
Polymyositis affects many different muscles, particularly around the neck, shoulders, back, hips and thighs.
Symptoms of polymyositis include:
muscle weakness
aching or painful muscles and feeling very tired
finding it hard to sit up, or stand after a fall
swallowing problems, or finding it hard to hold your head up
feeling unhappy or depressed
You may find it difficult to get up from a chair, climb stairs, lift objects, and comb your hair. The muscle weakness can become so severe that even picking up a cup of tea can be difficult.
The muscle weakness may change from week to week or month to month, although it tends to steadily get worse if you do not get treatment.
Symptoms of dermatomyositis
The symptoms of dermatomyositis are similar to those of polymyositis, but there's also a distinctive rash.
Before the muscle symptoms start, a red, purple or dark rash often appears. It is usually on the face (eyelids, nose and cheeks), and hands (knuckles). It can also sometimes be seen on the back, upper chest, elbows and knees.
The rash can be itchy or painful, and you may also get hard lumps of tissue under your skin.
Diagnosing myositis
A GP will ask you about your symptoms and examine you. If they think you may have myositis, you'll need to have some tests to help rule out other conditions with similar symptoms.
Tests you may have include:
blood tests, to check for raised levels of enzymes and antibodies in your blood
taking a small sample of muscle tissue or skin (biopsy) so it can be examined for swelling, damage and other changes
MRI scans
electromyography (EMG), where a small needle-shaped electrode is put through your skin and into your muscle, after a local anaesthetic, to record the electrical signals from the nerve endings in your muscles
Treating myositis
Exercise and physiotherapy
Exercise is a very important part of treatment for all types of myositis. It can help reduce swelling, give you more energy, and build up or restore your muscle strength.
Exercise and physiotherapy are particularly important if you have inclusion body myositis (IBM), as these are the only treatments for this type of myositis. IBM cannot be treated with medicines.
You should speak to a GP and physiotherapist before starting a new exercise programme for myositis. They will help to make an exercise plan that is right for you.
You must be very careful about exercising if you have severe symptoms of myositis, such as severe muscle pain and weakness (a "flare up"). Most specialists do not recommend exercising during this period.
But, it's very important to maintain gentle movement of your muscles and joints, especially if myositis developed during childhood. This makes sure that your joints do not become stiff and end up in a fixed position.
Steroids
Steroids are the main type of medicine used to treat polymyositis and dermatomyositis. They help to quickly reduce swelling and ease muscle pain.
They can be given as a tablet or injection, or directly into a vein through a drip. You will usually be given a high dose to start with, which is reduced over time.
High doses of steroids taken over a long time can cause side effects. These include:
weight gain
high blood pressure
diabetes
cataracts (cloudy patches in the lens of the eye)
osteoporosis (weakened bones)
Read more about the side effects of steroid medicines.
Disease-modifying anti-rheumatic drugs
If the swelling in your muscles flares up, your doctor may prescribe a disease-modifying anti-rheumatic drug (DMARD).
DMARDs, such as azathioprine, methotrexate, cyclophosphamide or mycophenolate, suppress your immune system and help reduce swelling.
These medicines take time to work, but in the long term, they may help you to reduce your dose of steroids. This can help ease the side effects of steroids.
Immunoglobulin therapy
Very rarely, you may need immunoglobulin therapy to stop your immune system attacking your muscles.
This involves having an injection of healthy antibodies (immunoglobulins) from donated blood.
Immunoglobulin therapy is given in hospital, usually directly into a vein through a drip. You may need more than 1 treatment.
Biologic therapies
Biologic therapies, such as rituximab, can also help manage the symptoms of myositis. They are widely used to treat conditions such as rheumatoid arthritis and psoriatic arthritis.
They help to reduce swelling and tend to only be used for severe myositis.
Outlook
Most people with myositis respond to a combination of steroid and immunosuppressive therapy, alongside carefully controlled exercise.
Steroids are often needed, in very low doses for several years, as well as medicines to suppress the immune system. This can lead to an increased risk of infection. In most cases this can be easily managed with antibiotics if it becomes a problem.
Complications of myositis
Some people with myositis do not respond well to treatment and find the condition significantly affects their everyday activities and quality of life. But continuing to exercise usually helps improve muscle strength.
If you have severe myositis, you may develop breathing and swallowing problems. Speech and language therapy may be recommended if you're having problems swallowing or it's affecting your ability to communicate.
In rare cases, myositis can be associated with cancer, and you may be offered tests to check for cancer.
Help and support
Myositis UK provides further information and support for people who are diagnosed with myositis and their families.
The Myositis Association (of America) also provides information about polymyositis and dermatomyositis.
1 note
·
View note
Text
I have a pt who was found down at home with multiple injuries. He had a seizure in the ED. EEG and MRI with and without contrast are pending. He keeps having low grade fevers, but his UA, CXR, and CBC are unremarkable for clear sources of infection. He has elevated CPK so it could be a result of his seizures. Maybe he's still seizing even though we have him on Keppra. We've been giving him fluids for the elevated CPK (rhabdomyolysis). We consulted Infectious Diseases and Neurology. It could be some kind of myositis. He had these ecchymoses on his eyelids. He has a history or RA as well! I went to UpToDate to review myositis:
The idiopathic inflammatory myopathies (IIMs) in adults include dermatomyositis (DM), clinically amyopathic DM (CADM), polymyositis (PM), overlap syndromes, antisynthetase syndrome, immune-mediated necrotizing myopathy (IMNM), and inclusion body myositis (IBM). (See 'Major disease subtypes' above.)
●An IIM should be considered in patients presenting with muscle weakness, most commonly gradual-onset symmetric proximal muscle weakness. Most patients will also have elevated muscle enzymes, with creatine kinase the most sensitive and most commonly tested enzyme. (See 'Clinical presentation' above.)
●Extramuscular presentations include a variety of cutaneous manifestations, interstitial lung disease, rheumatoid arthritis (RA), or Raynaud phenomenon. Features of overlap syndromes may also be present, such as findings of systemic lupus erythematosus (SLE) or systemic sclerosis (SSc; scleroderma). Patients with CADM and some with antisynthetase syndrome will present with only extramuscular manifestations and no evidence of muscle involvement. (See 'Clinical presentation' above.)
●Muscle enzymes should be obtained to aid with diagnosis. A panel of myositis-specific and myositis-associated antibodies may also be helpful. (See 'Laboratory findings' above.)
●IIM needs to be differentiated from other causes of proximal muscle weakness and rash, including hypothyroid myopathy, muscular dystrophies, metabolic myopathies, drug-induced myopathy, and SLE, among others. (See 'Differential diagnosis' above.)
●Treatment of IIM depends on the specific subgroup of IIM and should be individualized for the specific patient. Initial treatment usually includes glucocorticoids and glucocorticoid-sparing agents to suppress muscle inflammation and restore strength. Commonly used agents for IIM include methotrexate, mycophenolate, azathioprine, intravenous immune globulin (IVIG), and rituximab, among others. Skin disease in DM may warrant a different therapeutic approach than those typically utilized to target muscle disease.
2 notes
·
View notes
Text
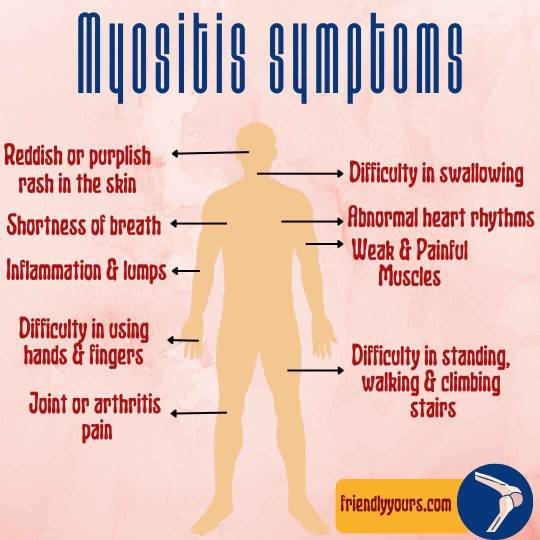
IS THERE ANY NATURAL TREATMENT FOR MYOSITIS? KNOW ITS CAUSES, SYMPTOMS, PREVENTION, & COMPLICATIONS
Myositis: Many people may not be aware of this disease. But recently this disease has become viral in social media as south Indian actress Samantha Ruth is diagnosed with myositis. Samantha is fighting myositis autoimmune disease confidently. Is there any natural treatment for myositis? What causes this disease?
How to know that we are having this issue? Are any preventive measures available? When to rush to the doctor immediately to avoid huge complications? Let us see everything in this article.
#myositis#myositissupport#health#raredisease#inflammatorymyopathy#youngadultsmyositis#myositisLIFE#MSU#Samantha#SamanthaRuthPrabhu#autoimmunedisease#Yashoda#raynaudsdisease#raynauds#ughcoldweather#dermatomyositisfighter#dermatomyositis#myositisawareness#myositislife#invisibleillness#invisibledisability#chronicillness#myositiscanada#neuromusculardisorder#nocure#invisibledisabilities#myositiscaregivers#dermatomyositissucks
1 note
·
View note
Note
Autoimmune culture is your medicine making you feel all sorts of wonky
Aaa
Ty for the message on the last ask, this is the same person! I'll probably be referring to myself as 🌞 anon
Relief will come eventually I hope
ooh yeah my meds also do that! i've never liked taking my immune suppressants, but it's at least worth it for less pain on my side
ofc! i love hearing from you and i'll keep trying my best to give encouragement!
#autoimmune culture is#dermatomyositis#chronically ill#immune suppressants#medication#illness tw#🌞 anon
5 notes
·
View notes
Text
Myositis (dermatomyositis & polymyositis ) - Treatment in India
Myositis refers to any condition causing inflammatory myopathies of the muscles & can be caused by injury, infection, or autoimmune disease. Call +91-124-4141414
0 notes
Text
that’s right people I will be attending the virtual support group meeting for my autoimmune condition this Saturday. That’s right don’t get too jealous of my plans 🤩
#mylife#chronic illness#Dermatomyositis#Lmao mainly bc I’m going to be starting a clinical trial soon and idk I want to talk to ppl who get where I’m coming from#Even if they are relatively older than me
1 note
·
View note